Contact Dermatitis
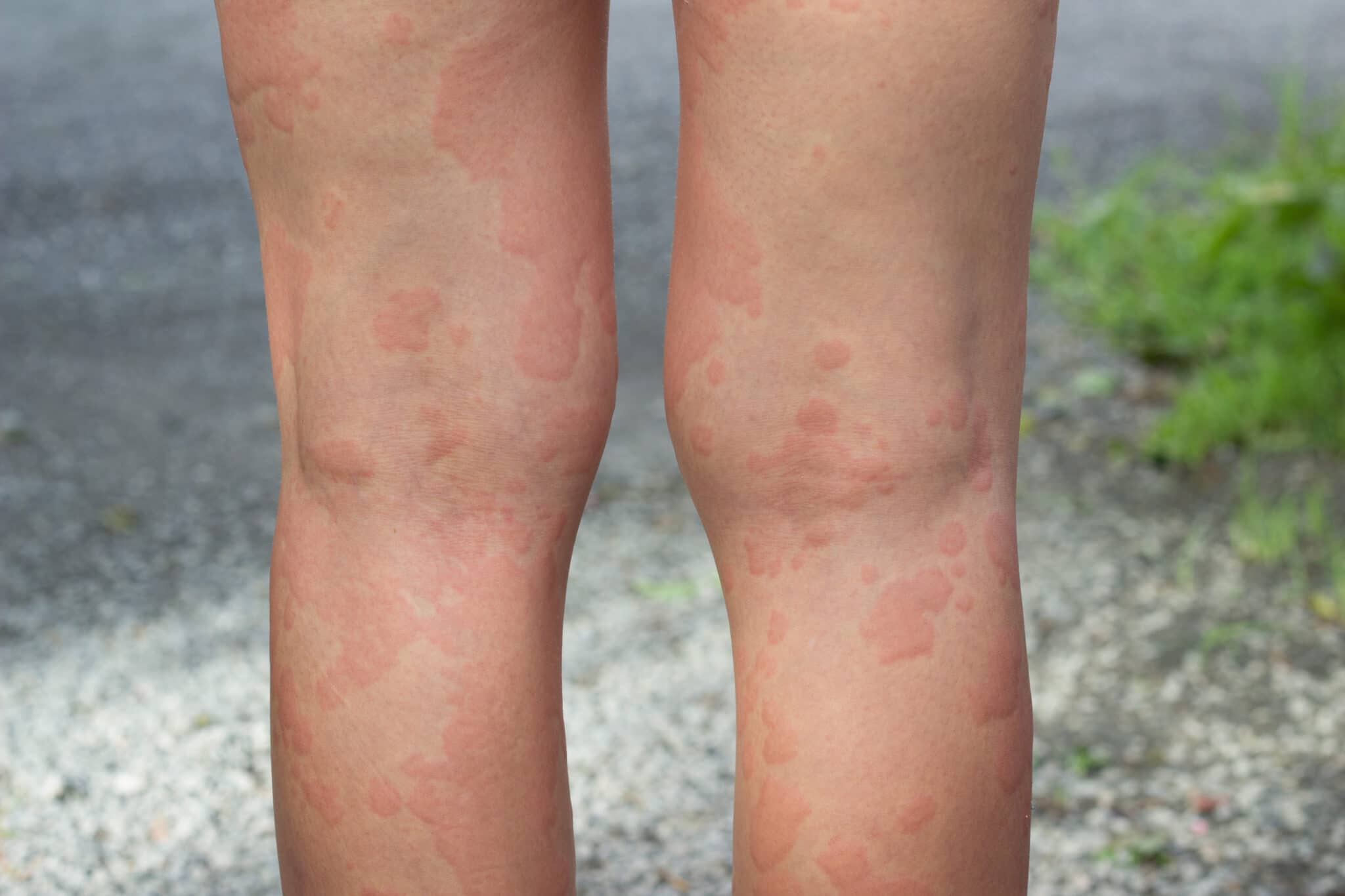
Understanding Contact Dermatitis
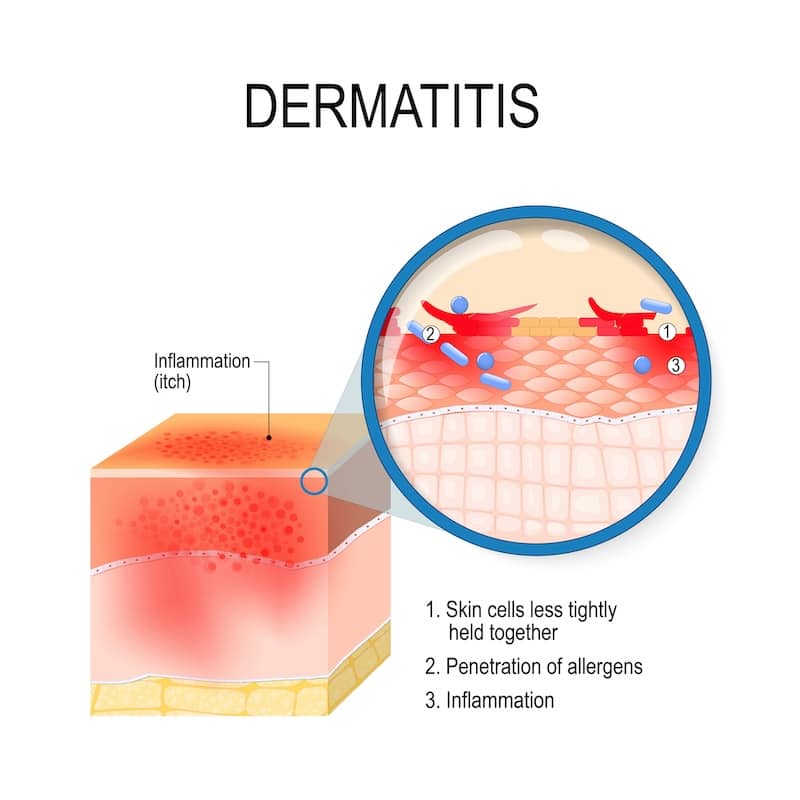
Contact dermatitis is a common skin condition characterized by inflammation resulting from direct skin contact with an irritant or allergen. It manifests as redness, itching, and sometimes blistering, and can affect individuals of all ages and backgrounds.
Types of Contact Dermatitis
Irritant Contact Dermatitis (ICD): This form is more common and results from exposure to irritating substances such as soaps, detergents, or chemicals. The severity often depends on the concentration and duration of exposure.
Allergic Contact Dermatitis (ACD): A delayed hypersensitivity reaction to specific allergens, ACD occurs when the immune system reacts to substances like nickel, poison ivy, or fragrances. The response may not appear until 24 to 72 hours after exposure.
Types of Allergic Dermatitis
Metals:
- Nickel: Found in jewelry, watches, and belt buckles, nickel is a common allergen. Contact with nickel-containing items can cause skin irritation.
- Cobalt: Present in certain metal alloys and pigments, cobalt can be found in industrial settings and may cause allergic reactions.
Poison Ivy, Poison Oak, and Poison Sumac:
- These plants contain an oily resin called urushiol, which can cause ACD in susceptible individuals. The reaction may include redness, blistering, and severe itching.
Perfumes and Cosmetics:
- Many fragrances used in perfumes, colognes, and cosmetics can trigger allergic reactions in sensitive individuals. Ingredients like essential oils and synthetic fragrances are common culprits.
Parabens:
- Widely used as preservatives in cosmetics, skincare products, and pharmaceuticals, parabens can cause ACD in some individuals.
Latex:
- Found in gloves, condoms, and some medical devices, latex allergy can lead to ACD. Symptoms may range from mild redness to more severe reactions.
Paraphenylenediamine (PPD):
- Present in many hair dyes, PPD is a common allergen that can cause allergic reactions on the scalp, neck, or face.
Disperse Dyes:
- Found in clothing and fabrics, disperse dyes can cause ACD, particularly in individuals with a sensitivity to textile dyes.
Bacitracin:
- An antibiotic used in some topical ointments, bacitracin can cause allergic reactions in susceptible individuals.
Oxybenzone:
- A common ingredient in sunscreens, oxybenzone can cause ACD in some individuals with sensitivity to this chemical.
Testing
Patch Testing: This involves applying small amounts of common allergens to the patient’s skin, usually on the back. The skin is then observed for reactions over a specified period, helping identify allergens responsible for ACD.
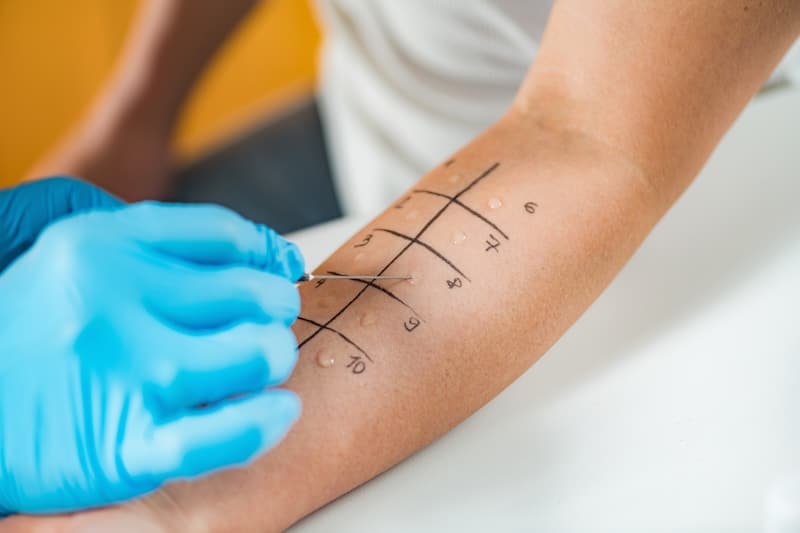
Skin Prick Testing: Commonly used for respiratory allergies, this test can also be adapted to identify contact allergens. Small amounts of allergens are applied to the forearm, and the skin is pricked to allow the substances to enter the epidermis, eliciting an immediate allergic response if present
Treatment Options
Topical Steroids: Mild to moderate cases often respond well to topical corticosteroids, which help reduce inflammation and itching.
Emollients and Moisturizers: Keeping the skin well-hydrated is crucial to prevent dryness and promote healing. Emollients soothe the skin and improve its barrier function.
Oral Antihistamines: These may be recommended to alleviate itching and improve sleep quality, particularly in cases of severe pruritus.
Avoidance of Triggers: Identifying and avoiding contact with the allergens or irritants responsible for the dermatitis is paramount to preventing recurrence.
Meet Our McGovern Allergy & Asthma Clinic Physicians
Contact Dermatitis News

Contact Dermatitis and Cosmetics
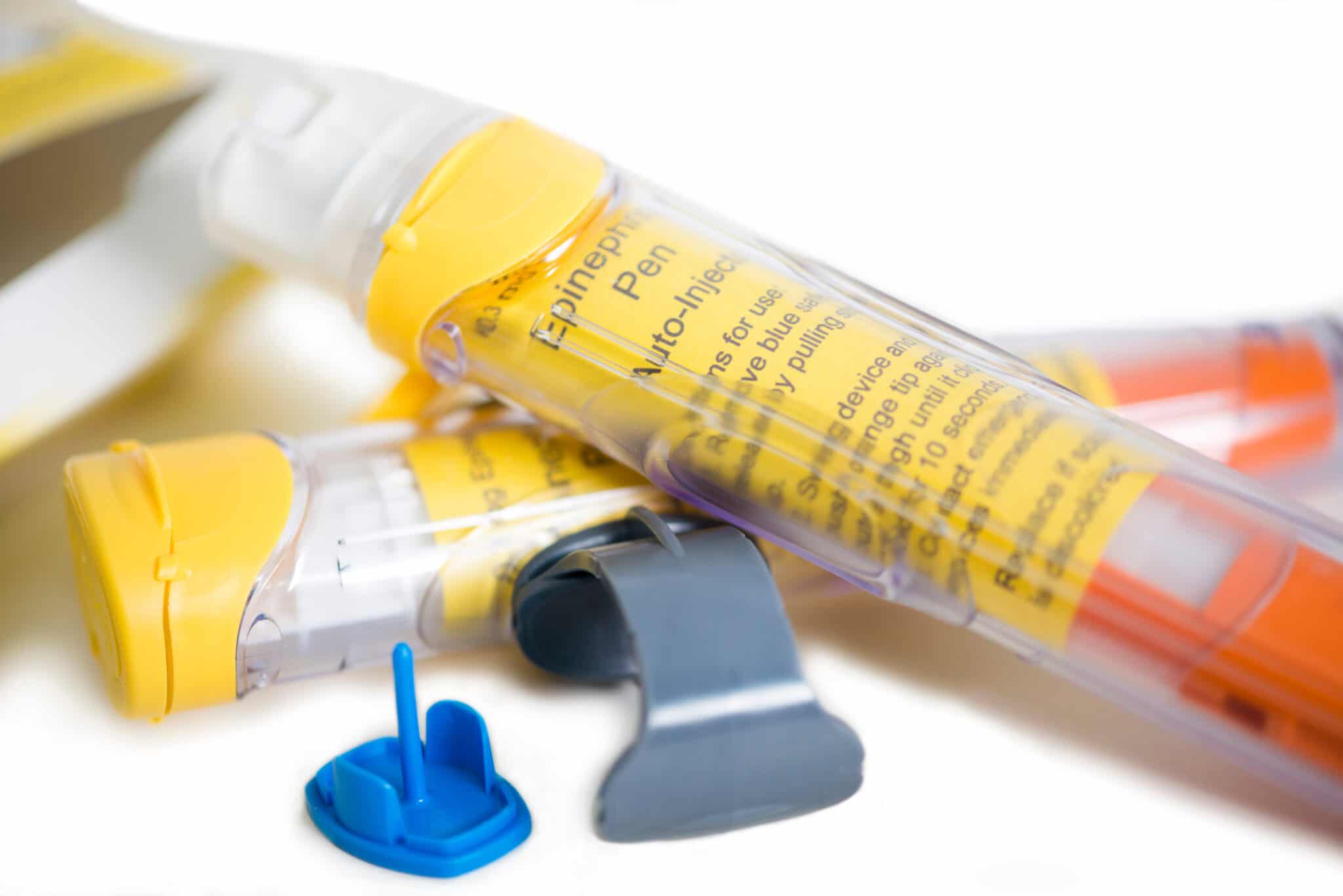
Epinephrine Autoinjectors: How and When to Use Them
Get the Most Out of Your Allergy Appointment: What You Should Know